Well, duh! If your back hurts it’s because it got hurt. Isn’t this pretty straightforward and evident?
Yes, and … no! Not really.
And before you say something along the lines of: “Of course! It’s because of a…” (Insert: weak core, tight psoas, muscle imbalances, or any other approaches that will be discussed in future installments) I want to clarify that—at least for this segment—I’m trying to keep it in a direct line with the back.
Yes, back pain is one of those pesky, overly common ailments that brings constant misery and costs Americans a significant chunk of revenue and productivity every year. Jacy Bryla of the Integrated Benefits Institute reports that low back pain can cost an employer up to $86,000 per 100 employees [1]. You can only imagine the combined costs of all work forces nationwide. However, despite its prevalence and the vast time and resources devoted to understand it, back pain mocks every breakthrough we believe it’s the holy grail of cures.
What is it about the back that makes it such a playground of ambiguities and frustrations for the world of therapy?
It is my professional opinion that as long as we keep focusing on the back itself as the source of its own issues, we’ll keep finding frustration.
The common procedure for back pain is to scrutinize it for deviations from established standards. Images and assessments search for bulging discs, narrowing of spinal canals, postural deviances, or weaknesses. When these anomalies are found, they’re likely to be catalogued as the source of the problem and efforts will be directed to correct them or eliminate them via conservative modalities. When conservative treatment fails, back surgery is seen as the final solution.
Unfortunately, the success rate of back surgery is less than stellar. From the simpler—if there’s such a thing in surgery—laminectomies and laminotomies, all the way to spinal fusions, we all know at least one individual whose high hopes in surgery turned into despair. A February 15th, 2011 study in the Spine Journal [2] reports that out of 725 cases of lumbar fusion, only 26% (or 188) returned to normal activities. Of that remaining 84%, a significant number experienced complications like permanent disability, more surgeries, and increased opiate usage. The success rate for other surgical procedures doesn’t fare too well either [3] leading to the now infamous FBSS or Failed Back Surgery Syndrome.
How is it possible? Didn’t the assessment and images show the abnormalities? Does that mean that all those assessments, MRIs, CT scans, and X-Rays are wrong?
Not at all—it just means that those abnormalities commonly blamed for back pain and dysfunction may not be abnormalities after all.
Take for instance, the well-conducted study published by The New England Journal of Medicine [4] where Magnetic Resonance Imaging (MRI) examinations were performed on 98 asymptomatic—as in going about daily life with no back pain—individuals. Out of this group, only 36% had discs that could be considered normal. The remaining 64% exhibited abnormalities ranging from minor bulging to significant herniation.
So, what do these findings mean to you?
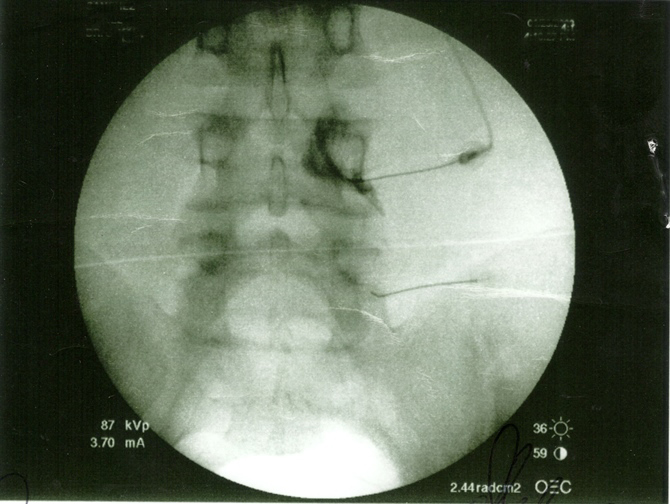
Probably the same thing they meant to the researchers: That the discovery of bulges or protrusions in people with low back pain may frequently be coincidental.
Read the study if you have doubts and you’ll know I’m not making this up. You will also realize that these observations are not recent. In 1990—yes, as in more than 25 years ago—SD Boden of the Department of Orthopaedic Surgery, at the George Washington University Medical Center, Washington, D.C. reported such findings [5] which in turn lead to further studies.
And the research continues strong. Dr. Michael Modic, chairman of The Neurological Institute at the Cleveland Clinic, has conducted several studies, including one with 250 symptomatic patients [6] who complained of severe back pain and pain radiating down the hips and legs. Dr. Modic did an initial imaging-scan and a follow up imaging-scan after six weeks.
His findings on patients who showed hernatiations were fascinating. In about 13 percent of those patients, the herniation had grown or a new one had appeared. On the other hand, in about 15 percent of those patients, the herniation had disappeared. This would not be a big deal save for two salient aspects:
- Dr. Modic found no relationship between the follow-up scan results and patients’ symptoms. Many of the patients whose herniations had disappeared still reported pain while many whose herniations had grown, reported improvement.
- Doctor Modic reported a consistent effect: When patients found out they had a bulging disc, their symptoms worsened.
While it seems logical that the back itself has to have experienced some direct injury that explains the root of the pain, reality shows us that the cause of back pain may not be as linear as we’ve been accepting for years.
And please don’t take it to the opposite extreme. A back injury should never be casually dismissed and if you experience severe symptoms—like losing bladder and bowel control, difficulty walking, paralysis, intense pain, fever, or nausea—you may require emergency surgery. While these extremes are rare, they must be respected and addressed with professional medical care.
The point is that while it’s tempting to blame well-known back structures for back pain, there are hundreds of other lesser known structures that affect the back directly but are rarely—if ever—taken into account.
If Not the Back, Then What?
What causes back pain, then? What keeps perpetuating the misery when the back itself has been ruled out?
The answer is: It depends!
If we stop obsessing on the back itself, then we may finally notice the hundreds of structures adjacent to the back, any of which could produce pain or dysfunction. No, I’m not talking about the core muscles. What I’m talking about is the vessels, ligaments, nerves, and linings—the deep fascia—inside the abdominal and pelvic cavities. While they receive little or none of the attention, they can react with protective reflex arcs and produce back pain symptoms.
Take for instance, the mesenteric root. This J-Shaped ligament—to which the small intestines attach to the peritoneum in front of the spine and in the right sacroiliac joint—can make it painful to straighten the body when standing up, or straighten the legs when laying down. Fascial-Counterstrain addresses this by shortening the mesenteric root, thus shutting off the protective reflex arcs. the image below illustrates the process.

Now, while the visceral ligaments are significant contributors in back pain and dysfunction, that doesn’t mean that every case of back pain is rooted in one of the many visceral attachments. Sometimes the dysfunction can be straight forward. Take for instance, the sacro-lumbar segment of the anterior longitudinal ligament. Fascial-Counterstrain treats this structure indirectly via positional finesse to shut reflex arcs off. The illustration below shows one of the areas affected by dysfunctions in this structure.
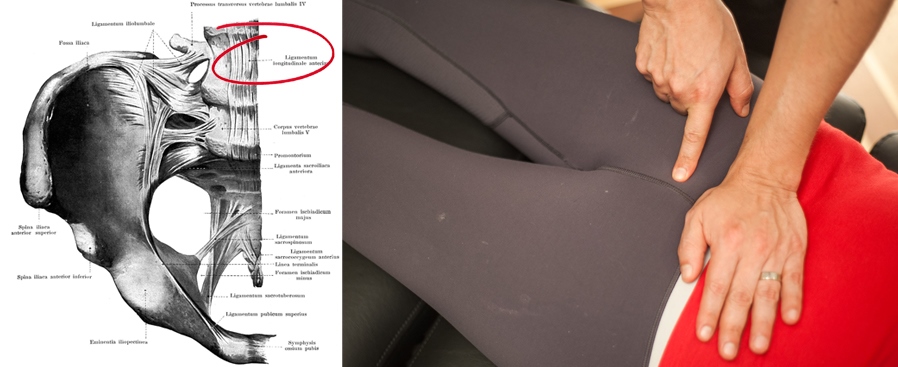
Incidentally, both the mesenteric root and the anterior longitudinal ligament produce symptoms that peg them as sacroiliac dysfunction. Not only does this blame the wrong structures, it also makes treatment ineffective, and occasionally counterproductive. My experience has shown me that trying to strengthen a sacroiliac joint that’s under the influence of reflex arcs in the the mesenteric root and anterior longitudinal ligament, only flares up the pain.
Is it a wonder looking for the root of back pain creates so much frustration?
Having a couple of so called abnormalities in our spines is nothing unusual, more so if we are in our mid 30s or older. It’s a normal part of living under the demands of gravitational forces and something the medical community is considering seriously before dictating treatment. I’m truly happy to see this.
If you’ve been dealing with the frustration of back pain and you’ve been treated with no success, it’s time to give Fascial Counterstrain a deserving chance. You’d be surprised at what the actual root might be.
Until next time, may you enjoy a fit and pain-free life!

References
[1] J. Bryla, “Low Back Pain Takes Toll on Worker Health & Productivity, Integrated Benefits Institute Study Finds,” 23 October 2013. [Online]. Available: https://www.ibiweb.org/community-events/low-back-pain-takes-toll-on-worker-health-productivity-integrated-benefits.
[2] T. H. Nguyen, D. C. Randolph, J. Talmage, P. Succop and R. Travis, “Long-term Outcomes of Lumbar Fusion Among Workers’ Compensation Subjects: A Historical Cohort Study,” Spine, vol. 36, no. 4, pp. 320-331, 2011.
[3] R. J. Gatchel, B. Miller and L. Lou, “Failed Back Surgery Syndrome,” Practical Pain Management, 1 May 2004. [Online]. Available: www.practicalpainmanagement.com/pain/spine/failed-back-surgery-syndrome. [Accessed 4 February 2016].
[4] M. C. Jensen, M. N. Brant-Zawadzki, N. Obuchowski, M. T. Modic, D. Malkasian and J. S. Ross, “Magnetic Resonance Imaging of the Lumbar Spine in People without Back Pain,” The New England Journal of Medicine, vol. 331, no. 2, pp. 69-74, 1994.
[5] S. D. Boden, D. O. Davis, T. S. Dina, N. J. Patronas and S. W. Wiesel, “Abnormal magnetic-resonance scans of the lumbar spine in asymptomatic subjects. A prospective investigation.,” The Journal of Bone & Joint Surgery, vol. 72, no. 3, pp. 403-408, 1990.
[6] G. Kolata, “The Pain May Be Real, but the Scan is Deceiving,” The New York Times, 9 December 2008. [Online]. Available: http://www.nytimes.com/2008/12/09/health/09iht-09scan.18514577.html. [Accessed 12 November 2015].
